 Just like birth – the journey of feeding your baby will be different for everyone. I asked some of my mums to share their feeding journeys to help to see the multitude of experiences and options when it comes to this part of your postpartum journey. Their stories include everything from the breast crawl, nipple shields, engorgement, lactation consultants, low supply, donor milk, colic, supply lines, expressing, bottle feeding, mixed feeding, formula feeding and more. I hope that by reading their journeys you will be able to connect with their experiences and feel less alone if you are finding feeding particularly challenging.
Just like birth – the journey of feeding your baby will be different for everyone. I asked some of my mums to share their feeding journeys to help to see the multitude of experiences and options when it comes to this part of your postpartum journey. Their stories include everything from the breast crawl, nipple shields, engorgement, lactation consultants, low supply, donor milk, colic, supply lines, expressing, bottle feeding, mixed feeding, formula feeding and more. I hope that by reading their journeys you will be able to connect with their experiences and feel less alone if you are finding feeding particularly challenging.
YOLLYS FEEDING JOURNEY
Before giving birth I made the choice that I would like to breastfeed. I was lucky to have a lesson with a midwife who was also a lactation specialist just before my baby was born. The main takeaway from that lesson was to allow my baby to find the breast on his own. It sounded a bit crazy at the time, I wondered how a fresh baby would make its own way to the nipple!? It worked though! Unfortunately a well meaning midwife placed my boy on the nipple the first time around but after that for the next few feeds I let my baby find his own way to the nipple from lying on my chest/stomach. It was made clear to me that the baby should latch after coming from below the boob, this way they open their mouth wide enough to get the whole nipple inside. Even though my baby had a tongue tie we never had any issues with his latch so we never had to get it cut.
I have one inverted nipple and found it quite painful for my baby to feed on this side (also the side the midwife placed him on, not sure if that is coincidence or just because of my nipple) so the visiting midwife suggested I use a nipple shield. This worked well as it relieved a little of the friction when my baby drew the nipple out.
For me breastfeeding hurt a bit to begin with. For a few weeks my nipples were quite tender. They say that it shouldn’t really hurt at all but I wasn’t in the habit of having someone suck on my boobs all day long before giving birth so I thought it was pretty normal to have a little pain (like chafing). This all subsided pretty quickly once my nipples became used to it. I’m really glad I have been able to breastfeed, sticking it out through those first few weeks of discomfort were worth it. Breastfeeding has been a lovely way for me to snuggle my baby who is otherwise always on the move.
TAYLOR’S FEEDING JOURNEY
Teddy made a spontaneous entry into the world at 31.5 weeks via natural birth.
Within hours of being earthside he was being fed small amounts of Donor Breastmilk, an option we consented to and feel very privileged was available to us, mixed with my colostrum via a tube. Once my milk came in, we were able to reduce the ratio of donor milk to my milk and within days I had enough to supply to support all feeds. At 36 weeks gestation Teddy successfully latched for a breastfeed first go and could soon do a mix of tube and breast feeds.
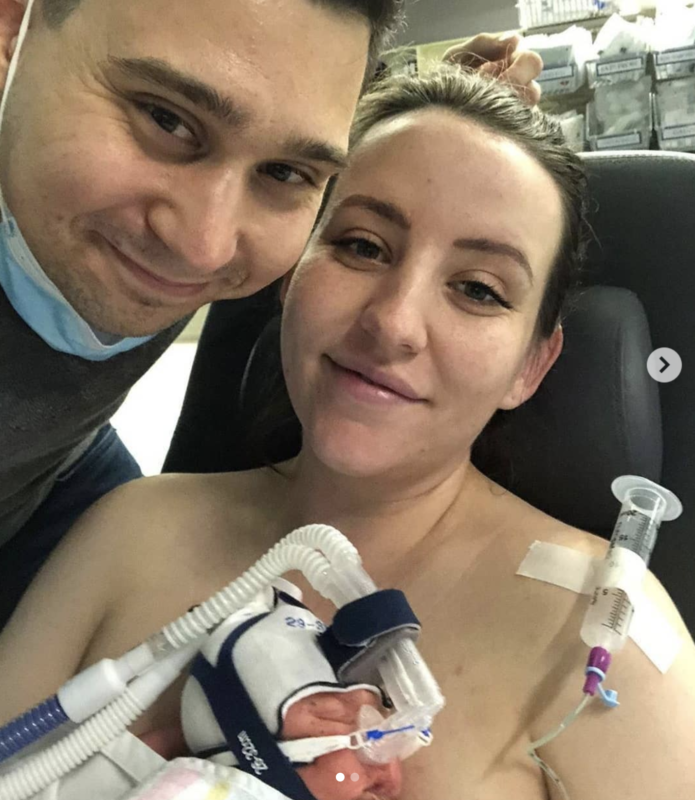
Before discharge Teddy had to be on all ‘suck feeds’ this meant a mixture of bottle and breast
feeds before they would allow him home. He favoured bottle feeds as breastfeeds were tiring at his size and he started to lose weight due to the physical exertion.
I felt immense pressure to breastfeed, it had been drilled into me in NICU that it was “liquid gold” and Formula was a ‘no go’. I wrestled with this for weeks after Teddy had come home, after months of 2 hourly feeds, pumping, 2x power pump sessions a day and my 100th bowl of oatmeal, I was EXHASUTED and felt like I was failing. Failing because my body couldn’t carry a baby to term and that it couldn’t sustain him. I couldn’t even cuddle him because if he was on me he wanted to feed and I felt resentful of my husband for their bond.
I was lucky to have a community nurse that did Teddy’s weigh in sessions 2x a week who could see the toll the pressure of not only keeping Teddy fed but also assisting him to gain large amounts of weight was having on me. I finally had the ‘permission’ I felt I needed, that I was longing for, to try formula.
When I finally made the decision to formula feed and wean, I felt like I could finally see Teddy and love myself as a mother. Motherhood didn’t need to be this chore of feeding, the never-ending power pumping sessions or filled with anxiety. I could remove all the stress and just feed him, love him and finally have delicious newborn cuddles!
“Breastmilk isn’t liquid gold if it costs you your happiness”
I’m hopeful to carry another healthy baby again.
I hope to give birth at full-term.
I’m also hopeful to be able to breastfeed or attempt breastfeeding again. I will go into that journey knowing that motherhood is so much more than how you feed your baby and hopefully with a little more kindness for myself.
JESS’S FEEDING JOURNEY
I thought the latch would hurt more but it was ok the first few days and gradually got more tender on the nipple as the feeding continued round the clock but was never painful in the way that I dreaded a feed – one upside was that I loved having bigger boobs lol! I didn’t know about the let down and how intense that could feel and the different way the baby sucked (true hunger vs comfort feed). I loved being able to stare into her eyes the more she woke up over the weeks (oxytocin is an awesome thing) – people said it would be tiring but I didn’t realise how long the feeds would be and the initial dependency of a newborn to want to be on you in the first few days – I remember thinking wow there really isn’t that much the partner can do at this stage.
Initially I used the standard hold then moved to holding her up higher so that she was more elevated for feeds – both my kids required elevation and to be held up 20 mins after a feed to help with their colic, unfortunately this lengthened the time I was awake for night feeds but it meant a more settled baby. No one told me how sore I could get in my shoulders and neck from holding baby for feeds and looking down at her, I consciously had to tell myself once she was latched, to relax my shoulders. By around week 3 or 4 things got easier as feeds got further apart and I started to see more baby cues. My partner helped to cook and provided emotional support. I loved that my babies could take the bottle, as this gave me flexibility when required and increased confidence of people being able to look after her when I felt I wanted to return to work. I introduced a bottle of breast milk at about 4 weeks then at 3 months introduced formula for the bedtime feed. I also like a social life so my babies being able to take a bottle of formula here and there was important for my self care – my SIL gave me loads of bottles that she had but what I quickly learnt was that she liked the teat that most resembled my breast – by 7 months she didn’t want the breast, loved being able to hold the bottle and fed herself with it which worked nicely as I returned to part-time work a few weeks later. I chose a formula for babies with sentitive tummies due to her colic. I quickly found out that persistent burping for colic babies was absolutely crucial for breast and bottle feeds.
KATRINA’S FEEDING JOURNEY
I gave birth at a private hospital in Sydney and before I gave birth quite a few people (Nat included) had told me to make the most of the breastfeeding support offered there during my stay. Great advice! I had no idea what I was doing initially and was struggling to get a good latch and finding it really quite painful, so every time Rosie wanted to feed I buzzed for a midwife so that they could check my latch and help me with positioning. There were lots of different midwives on duty over the few days I was there and they all had different tips which was good. I was taught the cradle hold, football hold and feeding while lying down. I went to an education session with a lactation consultant while there, who later did rounds of the ward to check how we were all doing. She was really great at normalizing that breastfeeding wasn’t always easy but that it would get easier and trying to explain the optimal positioning etc. I remember on my last day in hospital, a midwife came in to check on me while Rosie was feeding and on my chart she checked the box to say that she’d observed me feeding and that the latch was correct. It sounds silly but I remember feeling really proud.
Rosie was feeding well (lots of wet nappies; put on weight etc) but when I got home I was still finding it pretty painful. My nipples were cracked and so sore. I remember counting down the minutes, in agony and praying that Rosie would be finished soon. Lansinoh was an absolute saviour (this was actually one of the first things the midwives told me to do – she ordered Craig to go to the hospital pharmacy ASAP to get me the gel). I persevered and after about 7-10 days it suddenly stopped hurting. I’m not sure what changed; I think maybe my nipples had healed and Rosie had gotten the hang of latching well and I had gained some confidence. I then went on to exclusively breastfeed until just after Rosie’s 1st birthday.

I did bottle feed expressed breast milk too. I can’t remember when I introduced this, maybe around 8/9 weeks? I didn’t do it regularly in the early days as I was too lazy to pump and found it easier to just b/feed. I’d give a bottle if I was going out or wanted to have a drink. Because we didn’t do it regularly, sometimes Rosie would refuse it.. but by the time i went back to work (approx 9mths) Rosie was happily taking a couple of bottles of EBM a day. It was a bit of a punish to have to pump at work and to make sure that I’d have enough milk ready for my work days but it was only for a few months and a couple days/week. I did have a few hiccups along the way (engorgement, oversupply, mastitis and plugged ducts) – I found the ABA phone counsellors incredibly helpful and supportive. Eg first time I called I was engorged and she told me to hop in the shower straight away and hand express – instant relief! I called them a few other times for advice, and also visited my GP to get antibiotics for mastitis (which is so unpleasant btw, I was bed bound for a full day with flu like aches and pains)!
SARAH’S FEEDING JOURNEY
I’m coming up to 12 months of fulltime breastfeeding my beautiful little girl. Initially I had a lot of nipple pain and went through lanolin (which was ok), hydrogel breast dics (they are a bit chemical but create a nice cooling barrier) and an assortment of organic nipple creams. My favourite balm was hands down Moo Goo nipple balm. But my friend then put me onto Silverettes and they were an absolute game changer. They look a bit weird if you wear tight t-shirts, but I didn’t care. I wore them for a few months and loved them. I’ve had a pretty smooth journey. I was very scared about getting mastitis so was quite fastidious with cleaning anything that went on my nipples and massaging my breasts if they were getting very engorged during the first few months. For about 6 months I used the Haaka pump on alternate breasts and froze what I collected for emergencies. I freelance with my own business so have used the Spectra S2 breastpump on days when I’m out for work. The haaka only collects the thin top milk so the Spectra was my go-to for making sure I got thick milk with all the goodness. I love this pump. Having said that, my baby has never really taken to the bottle – so it’s more there so she has the option if I’m out. For the first few months, if I had to work all day, I’d always make sure I brought at least my haaka so I didn’t get too engorged throughout the day. I also highly recommend the Minbie steriliser and dryer, as well as Minbie bottles. Sarah
KAT’S FEEDING JOURNEY
I tried not to have too many expectations of what the first year of mothering might look like. But breastfeeding was definitely part of the picture – so much so that I had contacted a lactation consultant while pregnant to make sure I immediately had the right support. I had heard so many horror stories about bad latches, pain and struggles and I wanted to get on top of it as soon as problems emerged after birth.
After a straightforward pregnancy and an empowering birth (thanks Nat!), my daughter Cleo was placed immediately on my chest and I watched her as she crawled to my breast and sucked for an hour or so. Our breastfeeding journey was off to the start I had dreamed of.
The first two weeks were tough trying to get my small baby to open her mouth wide enough to get a deep latch. The seemingly inevitable nipple damage and grazes led to emergency midnight nipple shield purchases, calls to the Australian breastfeeding association hotline and googling different feeding positions with my husband in the middle of the night.
But I persisted and, with the help of a nipple shield and a helpful midwife who visited at home and suggested different feeding positions, my nipples healed quickly and things were looking up. When I went to my first community health clinic check up two weeks and two days after birth, I nodded with pride when the nurse watched me feed Cleo and remark ‘wow she knows what she’s doing. Look at her go!’
The nurse’s praise stopped there and then. Two minutes later she had weighed Cleo and was telling me Cleo’s weight gain was too low and that meant my milk supply was low so I had to go out immediately and buy a breast pump to stimulate supply and I also needed formula to top up. Well, that was unexpected. My alert happy baby was hungry and I hadn’t even noticed! Nothing quite like that wake up call to remove the spring from my step!
I was confident this was a short term issue we’d solve and I began working with a lactation consultant to get my supply up: feed on demand at least 10 times a day, pump as much as possible, switch feeding, breast compressions, taking medication (motilium) etc etc. I even went back to my obstetrician to have an ultrasound to check I didn’t have any retained placenta as that can be a reason for low supply. I had read that introducing formula top ups would undermine efforts to increase supply because babies get full on the formula and are therefore on the breast less. But, after the lactation consultant examined Cleo and commented on her saggy skin that wasn’t filling out, I had to introduce formula top ups to make sure she was getting food ASAP.
And so I fed and fed and fed. To get around the formula dilemma, I made sure I kept breastfeeding often and that formula was not replacing a feed but was always offered after as a top up. I also started using a supply line (supplementary nursing system) which allowed Cleo to get the formula top up through a tube attached to my breast. This meant she was still sucking (so stimulating supply) and had to work for her food – which wouldn’t have necessarily been the case if I had used a free flowing bottle.
After weeks of what felt like a rigorous regime, Cleo’s weight slowly increased but not enough to suggest the formula was no longer needed. My supply was still too low to exclusively breastfeed. I was in denial and kept reminding myself that so many of my symptoms were also experienced by mums who had enough milk – ie I didn’t leak much, I could often only pump drops, my boobs didn’t go from extremely full to empty following a feed, I couldn’t feel my letdown and so on.
I was pretty devastated. But what was more devastating was realising that I was actually devastated because my new mixed feeding regime did not align with my image of myself as some kind of mystical earth mama. So I didn’t feel guilty about giving Cleo formula but was more upset because not exclusively breastfeeding jarred with my identity. How vain and lame!
The lactation consultant told me she hasn’t had a case like mine in her 20 year career. It’s hard to know what to believe and I still do think low milk supply is super rare and usually a result of not feeding enough or a bad latch. I don’t know if there’s something I did along the way that was ‘wrong’ or if there’s another issue at play that caused my supply issues. We are now in the groove of mixed feeding and I hope we can do this indefinitely. Little Cleo is still in the 5th percentile for weight but tracking well and getting plumper by the day. She might just be a small kid, who knows. Someone has to be in the 5th percentile!
There are still a few terms that are anxiety inducing: deep, nutritive suck; 5-6 heavily wet nappies; fully drained breasts. These are the terms that governed my life for a couple of months. I’m grateful I can still breastfeed in some form or another and, of course, there are worse issues out there. But when you’re in the throes of first time motherhood and sleep deprived, the smallest things can feel like huge mountains of disappointment and struggle. I suspect there are a few more moments of struggle to rear their heads in my parenting journey!
MARILIA’S FEEDING JOURNEY
My baby was born at 40+5 weeks and I had a vaginal drug-free delivery, and for some unknown reason my body hasn’t produced enough milk.
My nipples were kinda short so it was hard for bubba to get a good grip and latch properly at first. So he hurt me, and by advice at the hospital we kept him off of the boob until I got to pump at least 30mls per breast, when we would start using a breast shield.
I was devastated when we left the hospital, but I was lucky my obstetrician had a lactation consultant at his clinic and she was able to talk to me since week 2, when I started taking on the herbs. We got to put baby back on my breast from week 3, and I also started on Motilium. All of it helped my supply to increase. At the end I was expressing 150ml every night.
And went on expressing, formula feeding and offering the boob for 6 months.
One thing that really helped to delay nipple confusion was the “pace feeding“. Baby started refusing the breast at some point and we tried using the Medela supply line (It was hard work and baby would get very agitated, so it didn’t work for us), but the feeding cup is what helped us get back on the boob.
For the last 2 months we’ve been only nursing and bottle feeding, but I keep avoiding using a dummy to keep baby interested in the boob as much as I can.
Under the advice of our consultant, we chose to use Aptamil as our formula brand as it is made from NewZealand’s milk (we should know where the milk comes from, she says).
Now, after 8 months these are the lessons I took:
– In our case, keeping baby off of the breast for more than 10 days was a mistake. We never got to use the shield and baby had no issues latching.
– Seeing a specialist was crucial to have tailored advice and start on the medications early
– Moogoo nipple ointment is the best! And the hydrogel discs make miracles too.
– Medication and herbs can help. But expressing and nursing are the most important – demand =supply.
– Breast is best but food is better!
Make your own choices, choose your battles and listen to your heart. So many people told me to give up, and here I am still nursing and giving formula on the side nearly 8 months on
AMY’S FEEDING JOURNEY
I never really thought about breastfeeding too much beforehand, but I had always just assumed I would breastfeed and that it would be second nature. When my first was born the nurses assisted me with every latch while in hospital. It was a massive help as it was a bit more complex then I had thought. My nipple still got damaged in those first few days and I used lansinoh and hydrogel discs frequently for the first few weeks (often together, keep discs in the fridge!). My boobs were so engorged and it was really painful but trying to push on the painful bits when feeding to release them did help a lot. I hadn’t considered the routine too much so it was an initial surprise to me when the nurse talked about feeding baby every 3-4hours (I guess I assumed the baby would just let me know when they wanted to feed). It is tiring and exhausting but it’s also really rewarding and pretty convenient once you get the hang of it. The nights were long and lonely at first (I tried to stay off my phone as it helped me to get back to sleep quicker after the feed). I think about 5 months I started to introduce a bottle of formula once a day just so I knew he could take something if I wasn’t around. He wasn’t a picky baby so he was happy to have any food/drink I would give him which made it easier. At about 10 months he self weaned from the boob and opted for 3 formula bottles a day. I was a little sad the journey was over but happy we got that far. I remember fretting a lot about the fact that you don’t know how much milk the baby is getting with breastfeeding- was he getting enough or not- You can’t control it and you can’t see it. He would cry quite a bit so i would question it often. But he always put on weight, so I grew to have confidence that my body was producing enough milk for him. My second breastfeeding journey was a lot easier as I had the confidence knowing I could do it and that I would have enough milk to meet their needs(twins). I did have to learn some new holds though (tandem football hold). Once every now and then I still tried to feed them separately just to get a bit more bonding time. It really is quite special.
WING’S FEEDING JOURNEY
I was lucky with breastfeeding. I took the Lansinoh Lanolin Cream with me to the hospital and used it religiously after every feed. I found it very soothing and more convenient than the gel discs as the Cream did not need to be removed before breastfeeding again, whereas the gel had to be removed. Using the Cream, my nipple pain lasted for a week or so.
The other thing I have loved is the Hakaa Breast Pump. Not only did this help me build up a milk supply for bottle feeds by popping it on the other boob with feeds, but it also helped me with engorgement as my baby reduced her night feeds by using it to release milk from both boobs when I woke up from them being too full and uncomfortable. I did find the Hakaa hard to fit on initially when my baby was small due to the cradle hold position, but it got easier as my baby got bigger and rested on the breastfeeding pillow.
Finally, I have had bad wrist pain from my baby lying on my arms when feeding. It has taken quite a long time for the pain to reduce, but to fix this, I have propped baby up high enough with breastfeeding pillow + extra pillow so that baby does not lie on my arm and I do not get a sore back from requiring to lean over.
 Just like birth – the journey of feeding your baby will be different for everyone. I asked some of my mums to share their feeding journeys to help to see the multitude of experiences and options when it comes to this part of your postpartum journey. Their stories include everything from the breast crawl, nipple shields, engorgement, lactation consultants, low supply, donor milk, colic, supply lines, expressing, bottle feeding, mixed feeding, formula feeding and more. I hope that by reading their journeys you will be able to connect with their experiences and feel less alone if you are finding feeding particularly challenging.
Just like birth – the journey of feeding your baby will be different for everyone. I asked some of my mums to share their feeding journeys to help to see the multitude of experiences and options when it comes to this part of your postpartum journey. Their stories include everything from the breast crawl, nipple shields, engorgement, lactation consultants, low supply, donor milk, colic, supply lines, expressing, bottle feeding, mixed feeding, formula feeding and more. I hope that by reading their journeys you will be able to connect with their experiences and feel less alone if you are finding feeding particularly challenging.
